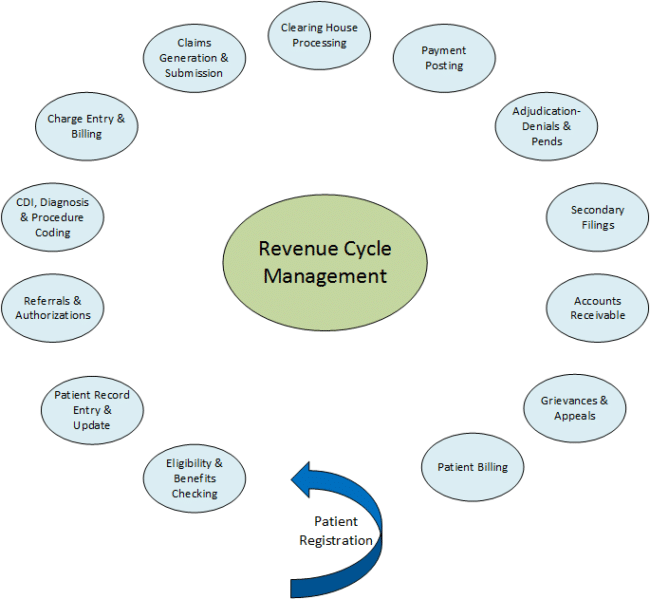
The last few decades have seen rampant changes in healthcare reimbursement. In 2018, healthcare spending in the U.S. skyrocketed to $3.65 trillion, firmly securing its distinction as the highest of any advanced economy. Unfortunately, these exorbitant expenditures don’t always equate to superior patient outcomes. The widening gap between the cost of care and actual care outcomes have resulted in several newly released programs and initiatives under the Affordable Care Act that redefined the reimbursement (and penalty) process for providers across the country.
Healthcare Providers Held to Different Legislative and Incentive Reimbursement Standards
These new legislative and regulatory initiatives mandate enhanced quality measures and utilization metrics explicitly designed to drive improvement at the practice level, reduce costs, and increase positive patient outcomes. In short, current legislation doesn’t allow provider reimbursement based on mere delivery of care alone. Instead, it’s shining a light on the overall quality of care that each patient receives, prompting practitioners to embrace a value-based care model within its facilities.
Practitioners Use Outside Resources to Transition to Value-Based Care
Unlike the standard fee-for-service model that incurs payment based on every medical transaction, regardless of outcome, the value-based care model is explicitly designed to control costs and improve overall quality of treatment received by patients. When appropriately implemented and overseen, a value-based healthcare approach helps establish nationwide standards of treatment accessible to all patients as well as helps reduce gaps in medical performance.
While most healthcare providers recognize the importance of increasing quality standards across every vertical and practice, many simply don’t have the resources needed to effectively, cohesively, and consistently transition to a value-based practice model. These U.S. providers are not only missing out on available reimbursement payments, but they also often find themselves facing fees, fines, and penalties for not maintaining the newly required standards of care and quality. As a result, practitioners nationwide are turning to outside healthcare resources to not only boost reimbursements and bottom-line revenues, but also recalibrate internal care standards, mitigate practice risks, improve workflow, and ultimately drive better patient outcomes.
Partnering with an outside provider to help transition to a value-based payment model that complies with all regulatory and legislative changes for optimized reimbursement delivers several crucial benefits, such as:
Full-Scale Implementation
Most healthcare practices and centers have several organizational segments, where groups, departments, and even entire locations operate in silos. An outsourced professional has the tools, technology, and talent needed to approach your medical facility as a whole entity. Your assigned team will systematically work through all relevant business intelligence to identify treatment trends, performance gaps, and missed opportunities, recommending changes for business process improvement and new strategic direction. Additionally, your consulting resource will also manage required system integrations for customized data visualization and dashboards that help leadership and stakeholders stay ahead of trends, patterns, and needed modifications.
Relieve Staff Obligations
Recent statistics show that the United States is on the cusp of a significant physician shortage, with many practices already feeling the pinch of reduced available resources. A report released from the Mayo Clinic revealed that more than 54% of physicians surveyed demonstrated at least one symptom associated with burnout. Put simply: today’s clinicians are overworked and overwhelmed trying to keep pace with an ever-increasing patient load.
An outsourced healthcare consultant reduces the responsibilities and stresses placed on existing internal personnel, particularly when dealing with the burden of clinical documentation requirements. An experienced consultant will streamline the entire documentation, minimizing staff obligation while maximizing reimbursement opportunities across each department. Additionally, your partner will keep up with any legislative and regulatory changes as needed, further lowering expectations on internal resources that are already spread too thin.
Organizational Training and Education
Most importantly, a qualified resource will not only manage reimbursement standards but also will conduct extensive training and education sessions throughout the entire organization. From leadership level seminars to ad hoc tutorials and refreshers, your consultant will work to fill informational gaps and ensure all relevant personnel operates from the same place of knowledge for sustainable, scalable results and success.
Contact InfoWorks Today
InfoWorks creates customized healthcare solutions that help providers in every vertical optimize efficiencies and standards throughout the entire continuum of care. Contact us today to learn more about our unique healthcare services and strategies.